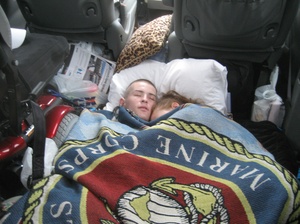
In a study of service members returning from Iraq and Afghanistan, researchers at the Rand Corporation found earlier this year that about 19 percent reported a possible traumatic brain injury while deployed, with 7 percent reporting a probable brain injury. An editorial last year in the medical journal the Lancet explained that due to increased use of explosive devices, the proportion of injured soldiers with TBI has increased to 60 percent, from 20 percent or less in previous wars. “With its mechanisms murky, diagnosis tricky, incidence under-reported, treatment uncertain, and personal, societal, and economic tolls enormous, TBI is a clear crisis for the U.S. military,” the editorial stated.
The results can be life-shattering. Even mild TBI, in which the victim never loses consciousness, can lead to erratic mood swings, impaired memory and confused thinking.
TBI used to be thought of as a single injury. But, over the past 10 or 15 years, a more complex picture has emerged.
“Now we know it’s a dynamic process,” said Dr. Ross Zafonte, professor and chair of the Department Physical Medicine and Rehabilitation at Harvard Medical School. “We like to separate it out into two parts.”
First is the immediate blow to the head. Neurons, the nerve cells that transmit and process information, might be stretched or torn apart entirely by the force. There might also be bleeding or swelling inside the skull, leading to more neuron damage.
But the process doesn’t end there. “There’s a whole chemical cascade,” said Lisa Kreber, senior neuroscientist and research coordinator for the Center for Neuroskills Clinical Research Education Foundation in Bakersfield, Calif.
“As neurons are damaged, chemicals and neurotransmitters get released in mass quantities. The blood-brain barrier might be compromised and calcium from your body could get into your brain. All that is toxic to brain cells, so you have further damage going on over the course of hours or days after the injury,” she said.
Trouble is, the damage isn’t always easy to spot. Axons, cable-like parts of neurons that form the fiber pathways information travels along, might not be completely broken, but could still be damaged from stretching and pulling. This kind of damage wouldn’t show up on an MRI or CT scan, Kreber said. So doctors might not realize anything is physically wrong.
But diffusion tensor imaging, a type of MRI, could change that by showing doctors the individual axon pathways. “You can see where the pathways have been stretched and where there are holes, so you have a better idea of how much damage has been done and to what parts of the brain,” she said.
Another possible diagnostic technique would sidestep imagery in favor of chemical analysis.
Serum biomarkers are substances, such as proteins or enzymes, which show up in higher-than-normal or lower-than-normal levels in the blood following specific types of damage. Hospitals already use a biomarker test to diagnose heart attack victims and researchers are looking for a way to make diagnosing TBI as simple.
“This is still in the research stage,” Bullock said. “But the idea is that you could take sample and know whether the person has had a brain injury, how severe it is, and whether there’s ongoing brain damage from hour to hour based on the biomarkers present in the blood.”
Once doctors know TBI has happened, treatment can begin. One of the most promising areas of research in treating TBI is in the field of neuroprotection, essentially finding substances that can protect neurons and give them an extra line of defense against secondary damage.
One example of neuroprotection comes from a study detailed June 27 in the Journal of Biological Engineering. Researchers Andrew Koob and Richard Borgens of Purdue University found that secondary damage might be lessened by giving victims an injection of polyethylene glycol.
Rats that got the injection within four hours of injury showed less behavioral impairment than those who didn’t get a shot at all or got one after that four-hour window. Because of the time constraint, this type of treatment would probably be most useful in situations where emergency personnel could reach victims quickly and give the injection before the patient ever reached a hospital.
Note this last warning. The techniques under study necessarily deal with rapid response and amelioration of the conditions in order to avoid TBI rather than the treatment of it. This is important. This means that in addition to training doctors at military hospitals, there will be required training of rapid reaction personnel, including but not limited to the Corpsman and medic.
This will be difficult, time consuming, expensive and risky. But it is worth it to protect the brain function of our warriors who have suffered battle space explosions. It would be sinful and criminal not to invest in this technology.
Faster, please.